Health
Supposedly harmless peptide may be linked to Alzheimer’s disease
New paper from UC Santa Cruz chemistry lab argues that efforts to develop treatments for Alzheimer’s should stop ignoring a short protein called P3, the ‘neglected cousin’ of amyloid beta

Billions of dollars have been spent on Alzheimer's drugs that target Amyloid beta.
Getty Images
Press Contact
Key takeaways
- A new culprit: While billions of dollars have been spent targeting Amyloid beta (Aβ) in Alzheimer’s patients, a newly reevaluated, shorter peptide known as P3 forms toxic clumps faster than Aβ and may also contribute to the disease.
- Explaining stalled progress: The overwhelming focus on Aβ, and the erroneous assumption that P3 is harmless and water-soluble, may explain why current Alzheimer’s treatments show limited success and fail to stop the disease’s progression.
While companies developing drugs to treat Alzheimer’s disease have spent decades and many billions of dollars targeting Amyloid beta due to its role in clogging patients’ brains with harmful deposits, a biochemist at the University of California, Santa Cruz, says the peptide has a smaller, overlooked “cousin” that could also be neurotoxic.
In a new commentary published in the journal ChemBioChem, UC Santa Cruz professor Jevgenij Raskatov points to peer-reviewed research that he and others have done finding that a shorter peptide can also form concerning microscopic clumps and fibrils. In addition, this peptide—known as P3—may interact with Amyloid β (Aβ) in ways that modulate its accumulation and toxicity, and may therefore also be a potential contributor to neurodegeneration.

“The P3 peptide is, most likely, not the innocent bystander it was commonly thought to be. There’s still more research to be done. But this could turn Alzheimer’s research on its head,” said Raskatov, whose lab researches amyloid peptides to discover new ways to block toxicity and inform better therapeutics for Alzheimer’s patients. “P3 is a distinct aggregating peptide that is itself potentially neurotoxic and may be contributing to Alzheimer’s disease.”
Limitations of targeting Amyloid beta
The disease is the world’s most common neurodegenerative disorder, afflicting about 35 million people globally and costing in excess of $800 billion annually. The patient estimate is projected to double by 2050. Meanwhile, the majority of the more than 400 clinical trials for Alzheimer’s drugs targeted Aβ and mostly failed—or showed only modest results while triggering serious side effects such as hemorrhages and strokes.
The Aβ peptide is produced when a much larger precursor transmembrane protein in the brain, called the Amyloid Precursor Protein (APP), is sequentially cleaved by the enzymes β-secretase and then γ-secretase. This produces peptides of varied length, with the ones containing 40 and 42 amino acids receiving the most attention. They are commonly referred to as Aβ40 and Aβ42—the latter peptide being substantially more aggregation-prone and toxic, and hence, the principal therapeutic target for Alzheimer’s drugs for decades.
Current treatments include cholinesterase inhibitors and N-methyl-D-aspartate (NMDA) receptor antagonists, which offer temporary relief of symptoms but do not slow the disease’s progression. Recently approved antibody therapies targeting Aβ, including Lecanemab and Donanemab, were designed to clear the beta peptide from the brain.
But Raskatov said they’ve shown limited success to date. “Progress has been extremely slow, and the current state of the art in Alzheimer’s therapy leaves much to be desired,” he said. “We need fundamentally new approaches to the problem.”
P3 a.k.a. ‘Amyloid alpha’
The P3 peptide is the alternative major processing product of the same Amyloid Precursor Protein being cleaved, but instead by the enzymes α- and then γ-secretase. Raskatov has dubbed this isoform “Amyloid α,” or Aα, to help avoid confusion with regard to its properties. Previous studies erroneously assumed, without verification, that this peptide was non-amyloidogenic, non-toxic, and water soluble, and so would eventually dissolve in the brain.
As a result, P3 went understudied and was subsequently dismissed as irrelevant to Alzheimer’s disease. But as a peptide chemist, Raskatov and members of his lab decided to interrogate convention. They published three major manuscripts over the past five years demonstrating unambiguously that P3 is at least as capable as Aβ of forming amyloid deposits—and producing them more rapidly.
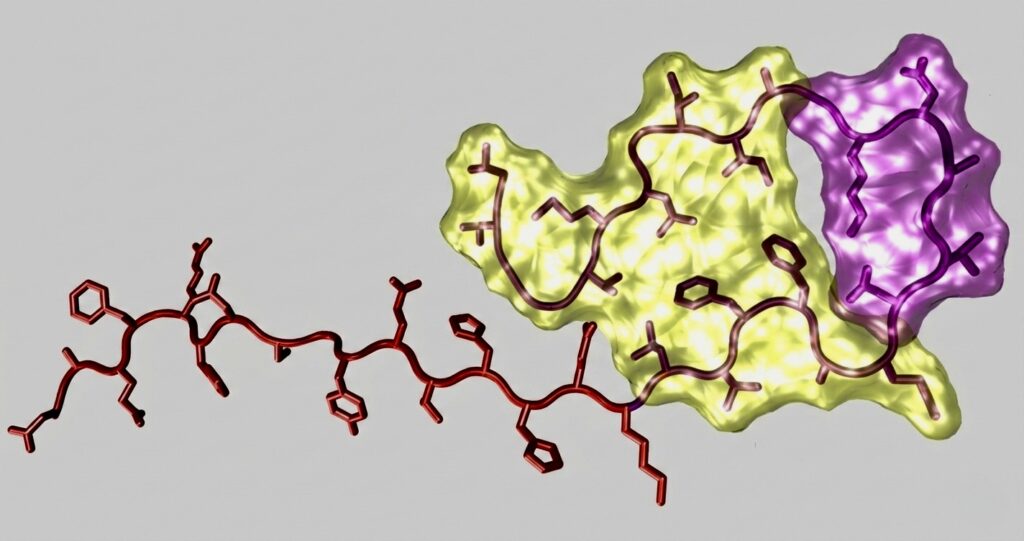
Finally, they found that P3 is itself potentially toxic to neurons, albeit less so than Aβ. Raskatov said their results were validated and extended by an independent laboratory in the UK, adding that studies from other labs aimed to better understand the interactions between Aβ and Aα are beginning to emerge.
Overcoming scientific dogma
David Teplow, an emeritus professor of neurology at UCLA and a leading Alzheimer’s researcher, said Aβ has been believed to be the culprit of the disease for decades. In an independent assessment of Raskatov’s work, Teplow said this is now changing.
“This reevaluation has far-reaching consequences for both basic science and clinical research into the causes and treatment of Alzheimer’s disease,” said Teplow, a founding editorial board member of the Journal of Molecular Neuroscience, the American Journal of Neurodegenerative Disease, and editor-in-chief of Progress in Molecular Biology and Translational Science.
When reviewing recent research by others, Raskatov said he has at times been quite shocked. He has found at least four scientific articles published in respectable peer-reviewed journals, citing his lab’s work as evidence that P3 is innocuous and does not form amyloid.
“This is exactly the opposite of what we have actually shown,” Raskatov said. “We remain in the dark on how this sort of grand confusion may have come about. Clearly, there is more work ahead of us.”